In modern dentistry, as in other branches of science, global changes are taking place. Today you are unlikely to feel pain in the dentist's office. In addition, modern methods of caries treatment do not require any use of drilling devices at all! Meanwhile, the final result of the work of a dentist who actually applies the latest developments in the industry will be much better and more durable. What is the paradox? Let's figure it out in order.
Modern methods of caries treatment
Unfortunately, all treatment methods without a drill are aimed mainly at combating the superficial form of caries. Their task is to stop the carious process that has begun, and in some cases, to prevent it. Before their appearance, treatment of dental caries was carried out only when it developed, and in the early stages it was simply not paid attention to.
The main advantages of modern methods are the absence of a drilling machine, as well as the ability to remove damaged tooth tissue without affecting its healthy part. So, the treatment of carious lesions without drilling is based on different principles of influence. Among the most common techniques in the newest dental industry: infiltration, ozone treatment of caries, air abrasive treatment and laser treatment of caries.
Modern technologies for effective caries prevention
E. A. Tyo
Doctor of Medicine, Professor, Head of the Department of Therapeutic Dentistry, Kemerovo State Medical Academy
In the structure of dental morbidity, dental caries occupies one of the leading places. The prevalence and intensity of caries among the Russian population reaches 99% [6]. The high incidence of dental caries is largely due to the peculiarities of their structure, function, the presence of microflora, and constant contact with oral fluid and food products [1, 11].
Experience accumulated in recent decades shows that the increase in pathology of hard dental tissues cannot be stopped solely by therapeutic measures [10, 27]. Therefore, all efforts of specialists should be aimed at preventing dental caries using innovative technologies and materials available on the global dental market and developed based on the results of evidence-based scientific research [2, 15, 16].
Currently, caries is considered an infectious disease, the likelihood of development and severity of which depends on many factors. In the modern understanding, the occurrence of caries is the result of a combined effect on the surface of teeth of bacteria and their metabolic products over a long period of time. The basis of the disease is the utilization of carbohydrates by the microflora of the oral cavity with the formation of acids. Practical implementation of the cariogenic influence of the main (but not the only) culprit of caries - Str. mutans - occurs through colonization in the oral cavity, carried out in the form of formation of dental plaque (in modern terminology, microbial biofilm). Dental plaque begins to form almost immediately after brushing the teeth, and its composition dynamically changes from the dominance of aerobic and facultative anaerobic forms, predominantly gram-positive cocci, to obligate anaerobic gram-negative rods and convoluted forms [4, 12].
It has been established that after ingestion of carbohydrate food in the oral fluid there is a sharp increase in the enzymatic activity of planktonic bacteria - a “metabolic” explosion, the basis of which is the activation of glycolysis. This leads to a sharp shift in pH to the acidic side due to the release of acidic catabolites - acetic, lactic, formic, pyruvic and other acids. In addition, the pH under the dental plaque decreases, and the process of demineralization of the tooth enamel begins. This occurs as a result of the ability of biofilm bacteria to accumulate excess carbohydrates in the form of reserve polysaccharides - dextrans and levans - with their subsequent metabolism, mainly through glycolysis, with the formation of organic acids. The structural elements of the enamel begin to lose ions, and a focus of demineralization occurs. Thus, the microbial biofilm initiates the development of the carious process [13, 21, 24].
Subsequently, the vital activity of the dental plaque microflora is successfully supported by the polysaccharides it stores for future use, which can be utilized, including between meals, ensuring the existence of microorganisms and the production of acids on the enamel surface during the entire period that the biofilm is on the tooth surface [14]. Taking this into account, the main etiological and etiotropically justified methods of combating dental caries should be the elimination of oral microflora pathogenic in relation to caries, reducing its quantity and cariogenicity, mainly by eliminating dental plaque and food debris. However, none of the methods existing today can achieve a significant reduction in the concentration of Str. mutans for a period of more than six months. Therefore, in order to select the most effective method of caries prevention, the prevention of plaque formation along with the removal of existing plaque is crucial [7, 30].
The main role in caries prevention continues to be the careful removal of dental plaque through regular tooth brushing. The goal of other measures for the prevention of caries, which are pathogenetically determined, is to give the hard tissues of the tooth greater acid resistance and stimulate their remineralization. Fluorides, including those included in oral hygiene products, successfully cope with this role. Fluorides can not only reduce the solubility of enamel in an acidic environment, stimulate remineralization, that is, influence the resistance of teeth to caries, but also inhibit the metabolism of plaque bacteria.
Fluoride ions can stop the enzymes that bacteria use to process sugars for energy. During this process, the formation of acids occurs, therefore, fluorides help reduce the production of acids. However, inhibition of bacterial activity occurs only in the presence of a high concentration of fluoride ions, which is impossible to achieve in the biofilm after using professional products and hygiene products containing fluoride. However, fluoride is the only clinically proven anti-caries agent used for routine use in oral hygiene products on a global basis.
Enamel behaves like a permeable membrane, and small ions penetrate into the depths more easily than large molecules that are adsorbed on the surface. In apatite, up to a third of ions can be exchanged. Penetration of substances into enamel and ion exchange occur in several stages. First, from the surface of the enamel, ions penetrate into the hydration layer of the crystal, from there to the surface of the crystal, and only subsequently from the surface to various sections of the crystal lattice. If the first stages last for several minutes and hours, then the last stage, the stage of intracrystalline ion exchange, lasts up to several months [1].
The possibility of remineralization of the focus of carious lesions in the initial stage of development of the pathological process (enamel caries in the spot stage) is due to the protective layer of calcium fluoride, which is a depot of fluoride ions in the oral cavity, from which fluoride is constantly released in small quantities. During acid attacks, the amount of fluoride released from the depot increases. The constant presence of fluoride in low concentrations in saliva enhances and accelerates the natural protective mechanism of remineralization [3, 5]. Thus, thanks to the remineralization process, the lack of minerals in the superficial localization of carious lesions can be replenished, caries in the spot stage can be stopped, and the tissue structure can be restored.
Fluorides increase the resistance of dental tissues to the demineralizing effects of acids and promote the processes of remineralization of hard tissues by retaining calcium and phosphates in close proximity to the tooth surface [5]. Compared to systemic fluoridation methods, recently more and more importance has been given to the application of fluoride-containing products directly to the tooth surface, including when using personal oral hygiene products. To date, literary sources are unanimous in the opinion that CaF2 temporarily becomes a reservoir of fluoride ions, maintaining a low concentration of fluoride in the oral cavity for a long time, including between hygiene procedures.
The main fluoride-containing compounds used in modern professional and oral hygiene products are sodium fluoride (NaF), sodium fluorophosphate (NaPO3F), sodium monofluorophosphate (NaMFP), aminofluoride (AmF).
The most important factor influencing the remineralization of enamel is also saliva. The physicochemical parameters of saliva are stable, which makes it possible to ensure homeostasis of the “saliva - dental plaque - tooth enamel” system. Mechanical brushing of teeth using toothpastes can be attributed to an external intervention in the oral ecosystem, which causes certain temporary changes in saliva. First, toothpaste works as an irritant, increasing the rate of saliva secretion; secondly, it contains chemicals, in particular fluoride ions, which temporarily become components of the oral fluid, inevitably affecting its composition and properties [3, 7]. Such parameters of oral fluid as a high secretion rate, a shift in pH to the alkaline side, a high concentration of total and ionized calcium and a relatively low content of organic phosphate characterize the saliva of caries-resistant individuals [1].
For the prevention of caries, conservative and minimally invasive technologies are currently in demand that promote the remineralization of early carious lesions and the elimination of the carious process at a very early stage [20, 25]. In particular, such technologies include a probiotic approach to caries prevention, implemented through the use of arginine, which complements the traditional effect of fluorides [26].
Arginine is a naturally occurring amino acid that is an essential building block for cell growth and is normally present in saliva. Arginine is a natural component found in many foods. The US Food and Drug Administration (FDA) classifies arginine as a GRAS (Generally Recognized as Safe) ingredient for use as a food additive.
The principle underlying the new caries prevention technology allows modulation of plaque pH by using the arginine deaminase enzyme pathway in non-pathogenic, arginolytic microorganisms. Arginolytic bacteria are able to break down arginine into ammonia, which neutralizes plaque acids directly in its matrix, stabilizing the microbial biofilm [8, 23].
Clinical studies have shown that exogenous sources of arginine can affect the activity of the arginine deaminase system. In a group of people brushing their teeth twice a day every day for four weeks with toothpaste containing only arginine, due to increased activity of the arginine deaminase system, the risk of caries decreases, which is comparable in effectiveness to fluoride-containing toothpaste [18].
The action of fluorides is concentrated on dental tissues as a means of controlling damage after the onset of the carious process, and arginine affects pathogenic plaque and prevents the onset of the carious process [22].
Since the mechanisms of action of arginine and fluoride complement each other well, a new generation of oral hygiene products has been created that combines arginine, an insoluble calcium compound and fluoride - a toothpaste containing 1.5% arginine, a calcium compound and 1450 ppm fluoride.
The action of toothpaste based on the “sugar acid neutralizer” technology is aimed at neutralizing acids directly in the plaque biofilm as the main cause of caries, and is also supplemented with the main benefits of fluorides. Using modern and traditional methods of caries detection, it has been clinically proven that toothpaste based on this technology can provide more effective caries prevention, reducing the formation of new cavities by 20% compared to toothpaste containing only fluoride.
The effectiveness of toothpastes containing 1.5% arginine, a calcium compound and 1450 ppm fluoride has been confirmed by eight years of clinical studies involving 14,000 people [9, 17, 19, 28, 29, 31, 32].
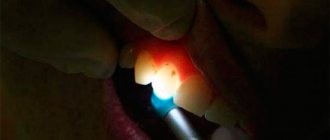
One of these studies in Chengzhu (China) involved 463 schoolchildren aged 9–13 years with initial carious lesions of the teeth. To detect and evaluate carious lesions, including long before the formation of a cavity, one of the most modern caries diagnostic methods was used - QLF (quantitative light-induced fluorescence) [13, 29]. Over the course of six months, changes in initial caries were recorded in children randomly divided into three groups that had no statistically significant differences in baseline data and used arginine-containing toothpaste and two control products. The positive control is a silica-based paste containing 1450 ppm of fluoride in the form of sodium fluoride, the negative control is a fluoride-free product. After six months of twice-daily brushing, improvements from baseline in ΔQ (lesion volume) were 50.6%, 34.0%, and 13.1%, respectively, for the novel arginine toothpaste, positive control, and negative control groups. . The difference between the study group and the positive control group was statistically significant (p = 0.003), as well as the difference between the negative and positive control groups and the study group (p < 0.001), which suggests that the identified differences in the data obtained are not random and , therefore, are reliable. [31]. This suggests that the new toothpaste, containing 1.5% arginine, a calcium compound and 1450 ppm fluoride, was more effective in inhibiting the development of caries and promoting the reversal of early caries lesions compared to a regular toothpaste containing only 1450 ppm fluoride.
Another larger, longer-term, double-blind, randomized, controlled, parallel clinical trial involving 5,559 participants showed similar results. Two years of observation showed that two toothpastes containing 1.5% arginine and 1450 ppm calcium fluoride, one with dicalcium phosphate and the other with calcium carbonate, were significantly more effective in preventing cavities than toothpaste containing only 1450 ppm fluoride. Three trained and calibrated examiners examined the baseline status of children aged 7–12 years, repeating the study one and two years later. In three groups of study participants randomly assigned to different toothpastes, the numbers of caries-affected, filled, and removed teeth due to complications of caries (CPUz) and surfaces (CPUp) at baseline were almost the same, with no statistically significant differences between groups, as well as after one year of use. However, after two years, children using toothpastes containing 1.5% arginine, a calcium compound and 1450 ppm fluoride had statistically significant (p < 0.02) lower CBF values (21.0 and 17.7% reduction, respectively). ) and KPUp values (16.5 and 16.5%) compared to the control dentifrice without arginine. The differences between the two groups using the new teeth cleaning products were not statistically significant.
Nowadays, the population is quite well motivated in matters of oral hygiene, does not lack a choice of hygiene products and usually chooses toothpastes containing fluoride. However, the problem of caries is still relevant. The advent of arginine-containing toothpaste makes it possible to maintain the acid-base balance of the oral cavity at normal levels, making the intraoral environment safe for the mineral components of enamel and unfavorable for cariogenic bacteria, and provides a new chance for more effective caries prevention, increasing the potential for the action of fluorides.
Infiltration method
Infiltration technology was invented at the Celtic University of Germany. This method of microinvasive treatment of caries refers to chemical-mechanical treatment, which completely eliminates tooth preparation - drilling, and is used only in the treatment of initial caries, initial carious lesions after using braces, as well as caries in the spot stage.
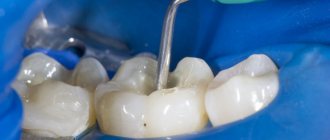
The principle of operation of the method is to apply a special gel to the surface of the affected area of the tooth, which splits the enamel, after which the carious lesion is dried with 99% ethyl alcohol in combination with an air stream and impregnated with a polymer resin.
The positive aspects of this technology can be considered painless and quick (the procedure takes 15–20 minutes) removal of exclusively the affected part of the tooth. However, the method is applicable only on the smooth surface of the teeth or between them. Also, the shape of the “hole” should be ideal - with smooth edges and a wide entrance. International studies have confirmed the effectiveness of the infiltration method, which has made it possible to stop the development of caries for many years in both adult patients and children.
Chemical-mechanical method
The chemical-mechanical method of caries treatment is considered the most common and painless. This method is based on the following technique: a special gel must be applied to the damaged area of the tooth, which contains substances that help soften enamel and dentin. Then the dentist must use a dental instrument to remove the softened affected areas, getting rid of caries.
It is also worth saying that the chemical-mechanical method is not suitable for all patients. Because if the tooth canal is tortuous, it will not help. Therefore, in any situation, the dentist should select a treatment method.
In order not to treat caries, it is better to prevent it, and for this you need to regularly visit the dental office and maintain oral hygiene. If you have any questions, you should consult a doctor and do not self-medicate.
Ozone treatment method for caries
Ozone therapy was developed in Germany. Unlike other modern methods of treating initial caries, the ozone method is aimed at suppressing tooth-destroying bacteria and subsequent remineralization of dental tissues. But it also allows you to avoid drilling, and therefore anesthesia. In some cases, it is possible to do without a filling!
The essence of the method is this: a special device converts oxygen into ozone, which instantly neutralizes carious lesions and destroys harmful bacteria that provoke the destruction of dental tissue. Then it “comes out” of the tooth, again being converted into oxygen. Healthy cells remain unaffected, as they are more resistant to oxidation and can withstand the effects of ozone. The procedure lasts about 20 – 40 seconds.
Who can be recommended for caries treatment with ozone? Almost any patient with the initial stage of caries, because ozone cannot cause allergic reactions, as well as irritation of the oral cavity. But if a deep carious process is observed, then you will still have to resort to drilling. In addition, ozone treatment is recommended to everyone without exception as a preventive measure for caries in adults and children.
What is caries?
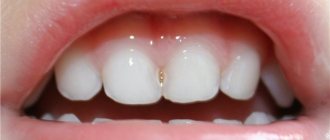
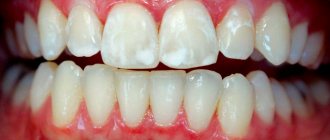
When you eat food, plaque forms on your teeth. During the cleaning process, some of the plaque is not completely removed (only professional cleaning can help with this). Under the remaining plaque, bacteria and microorganisms begin to actively multiply. During their life, organic acids are formed that damage the enamel. Tooth enamel loses its strength, becomes porous, and a white spot forms. The first stage of destruction is considered to be the appearance of such stains on the teeth.
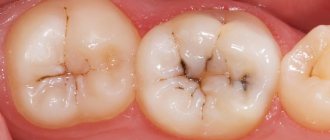
If the tooth is not healed at this stage, then deformations occur on the surface. They are carious cavities of varying depths.
Air abrasive processing
The air-abrasive method involves mechanical treatment of carious lesions using special sandblasting machines, which are also used for professional oral hygiene. The idea of “knocking out” superficial caries with a stream of air containing impurities arose in the 40s in the USA. Then quartz sand was used as an abrasive (an impurity with high hardness), and later - aluminum oxide, a colorless and non-toxic substance.
Flow-abrasive systems “shoot” with enough power to remove softened, caries-affected tissues without harming healthy ones. In the case of using air-abrasive treatment, the possibility of developing secondary caries is practically eliminated. The procedure is safe, painless, and does not require anesthesia when treating initial caries.
As with other methods of treating caries without a drill, the air-abrasive method does not heat the dental tissues and does not create noise or vibration. Moreover, it reduces the risk of microcracks forming, which can later cause destruction of the entire tooth. “Knocking out” with an air stream with abrasives occurs pulsed, for 5–10 seconds, which is more effective than dissection with a drill.
The air-abrasive treatment method is not ideal, because in some cases it may still be necessary to clean out the caries with a drill and place only a composite filling. Sometimes this treatment method is not applicable at all due to the inaccessibility of the installation tip to the affected area. Another disadvantage is the possible increase in tooth sensitivity in the future.
How is caries treated at the dentist?
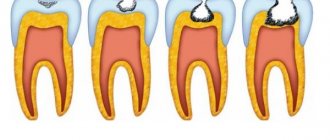
The treatment method for caries largely depends on its stage - carious spot, superficial, medium or deep.
Treatment of the disease at the carious stain stage is not very difficult. Usually it is enough to carry out a tooth remineralization procedure. In other stages of caries, much more manipulation is required to repair the damage in the tooth.
After the patient comes to the dentist, the doctor invites him to sit in the dental chair. Then the dentist examines the oral cavity and notes the condition of the teeth. If some teeth are affected by caries, the doctor suggests the patient to treat them. If there are several such teeth, then treatment usually begins with those where caries is most dangerous and has reached the most severe stage.
Nowadays, in almost all dental clinics, caries treatment is carried out with anesthesia. An exception is made only for pulpless teeth (those where the nerve bundle responsible for tooth sensitivity has been removed). Some patients may also be allergic to painkillers. For anesthesia, before starting treatment, the doctor injects an anesthetic into the gums.
After the tooth loses sensitivity, the doctor begins work. Before starting all procedures, it is necessary to isolate the diseased tooth from the rest and from moisture getting into it. For this purpose, special techniques are used, for example, laying an insulating rubber dam.
Only after this the doctor takes up the drill - the main tool in treatment. With its help, areas of the tooth affected by caries are removed. Also, the purpose of treatment with bur is to create a cavity into which a filling can be inserted.
After the cavity is created, it is disinfected. Typically, a 2% chlorhexidine solution is used for this purpose. The internal surfaces are then coated with an adhesive material. If the carious cavity is located close to the pulp chamber, then an insulating gasket is installed. Then a filling is installed. The last stage is grinding the filling. The doctor may ask the patient to bite on a special piece of paper to check if there is discomfort in any place when biting. If this is the case, then excess pieces of the filling are removed.
Laser treatment of caries
Treatment of caries with a laser, in other words, laser fluorescence, as well as the above methods, implies the treatment of caries without drilling in the sense in which we are accustomed to understanding drilling and the associated discomfort. Why does unpleasant pain occur while the drill is working? The fact is that intense heating and friction occurs between the dental drill and enamel, dentin. And to these sensations is added vibration that spreads to the dental tissues.
During laser treatment, tissue heating does not occur due to the low radiation power. In addition, laser devices are 20 times quieter than a drill! In this case, the main thing is not to accidentally fall asleep in the dentist’s office. It is not without reason that this method is recommended not only for people with increased sensitivity to pain and sounds, but also for those most sensitive to the perception of external stimuli - pregnant women and children. In addition, the procedure for laser treatment of caries is absolutely sterile - the tip of the laser unit does not come into contact with your teeth.
The laser performs cavity preparation by selectively affecting caries, or, more precisely, only tissue infected with caries. The impact completely suppresses the growth of carious bacteria and eliminates the risk of secondary caries. At the same time, the laser method does not harm healthy teeth, and also does not lead to microcracks in the enamel.
And the time spent on treating caries is reduced by about 40% compared to traditional treatment - there is no need to change attachments, and when treating superficial caries, there is no need to use anesthesia. Today, dentistry uses lasers not only as a method of treating caries, but also as a diagnostic method. The second is a significant advantage compared to X-ray diagnostics, since in the case of laser “checking” there is no radiation.
However, such a modern dental caries treatment method as laser exposure also has significant disadvantages:
- high demands on specialists working with lasers;
- such treatment requires the use of protective dark glasses by both the patient and the doctor;
- glasses with tinted lenses can distort reality and reduce the clarity of vision;
- in some cases, soft tissue damage caused by lasers heals slowly and poorly;
- There is also a possibility that the laser will reflect off metal objects in the dentist's office if they are not removed, causing a fire.
Nowadays, there is a lot of debate about how to cure tooth decay without pain and fear. Technologies that can solve dental problems without the use of a drill are just beginning to appear on the Russian market. In any case, even such modern methods of caries treatment are applicable in the early stages of its occurrence.
Therefore, if you are not eager to experience the effects of drilling with a bur, do not neglect the health of your teeth and seek help from specialists in a timely manner.
Treatment with laser
Operating principle
Dentists are increasingly using erbium lasers to treat caries and other dental pathologies. The length of the laser beam is adjusted so that it does not penetrate too deeply into the tooth tissue and overheat it.
Laser treatment
During laser treatment, the doctor removes areas affected by caries, having previously prepared the tooth surface using an ultrasonic scaler - a medical device that removes plaque. Under the action of the laser, unnecessary tooth tissues crumble and are washed away with a stream of water, while healthy ones remain untouched. Cleaned carious cavities are filled with a special adhesive system, which improves the attachment of the filling material and preserves the tooth structure.
Advantages and disadvantages
Among the advantages of laser treatment of caries is the absence of pain, noise, and vibration. Such treatment eliminates the occurrence of pulp inflammation and the formation of microcracks in the enamel. The laser beam sterilizes the treated area, destroying harmful bacteria. In addition, it increases microcirculation in the dentinal canals, due to which the tooth tissues increase resistance to caries. Laser treatment is fast, allowing you to treat several teeth at the same time.
Erbium laser treatment has no contraindications, so it is suitable for both adults and children. It can also be used by women at any stage of pregnancy.
Laser processing has two significant disadvantages: high cost and a long search for highly qualified personnel who have undergone special training. In addition, when working with a laser, it is necessary to carefully follow certain safety rules, for example, wear safety glasses and not leave the laser unit turned on unattended. The laser does not treat deep caries.
Do caries need to be treated?
Caries, does it need to be treated ? When asking dentists this question, the answer is yes. If caries is diagnosed at an early stage, dental health can be restored and improved in a short time, no more than two days. At this stage, the clinical picture is poorly expressed; only a specialist is able to detect the beginning process of tooth decay. If a change in the color of the enamel is detected, the dentist, using special tools and equipment, will saturate the damaged enamel with useful elements such as calcium and fluorine.
It is better if caries treatment is carried out precisely in the first stages of caries development, this will allow the dentist to use more gentle treatment methods, and will also prevent further tooth destruction. In the absence of therapy, caries progresses to the superficial stage, and then to the deep stage, which requires more powerful treatment methods, such as the use of a drill. Modern methods and means allow the procedure to be carried out as painlessly and quickly as possible.
It is very important to visit the dentist regularly, at least once a year, since more complex types of caries occur when destruction occurs under the filling, which can be caused by a number of reasons. In order to accurately assess the situation, diagnostics are prescribed before therapy, in particular an x-ray that determines inflammatory focus.
Principles of treatment
Today there are two main approaches to caries treatment:
- without the use of boron (preparation);
- with preparation, when the affected tissues are drilled out.
The first approach is also called conservative therapy or invasive treatment. Its use is suitable for the treatment of initial forms of caries, as well as in the presence of a cavity.
The approach to treatment using the preparation method has several stages:
- First, the oral cavity must be prepared for the procedure. It may be necessary to remove plaque and tartar from the tooth and have all teeth professionally cleaned.
- Use of anesthesia if necessary. This is most often local anesthesia, but there are cases (panic fear of small children, multiple lesions of the teeth in the oral cavity, etc.) when general anesthesia is used.
- Then they move directly to preparation. Damaged tissue is removed from the cavity formed by caries and treated with special medications. In this way, it is possible to create conditions under which the growth of bacteria under the filling and its loss are prevented.
- Next, the cavity needs to be formed so that it can hold the filling well. Sometimes it needs to be given a special configuration so that the filling compound does not fall out. But most modern composites do not require such mechanical retention, since they are able to contact the tooth chemically.
- Insulation padding may be required. This is especially important when treating deep-stage caries. Thus, the nerve has an additional effect that protects against germs and inflammation. The gasket prevents the filling material from irritating the nerve.
- Application of a filling. First, the doctor selects its color, then isolates the diseased tooth from the rest of the oral cavity using cotton swabs or rubber dams, then applies the composite in layers. To do this, they often use such auxiliary tools as a matrix to create a gap between the filling and the adjacent dental organ, wedges that form an ideal contact point, and a retraction thread to correct the gums near the working area.
- At the final stage, processing is done. The filling is adjusted according to the bite to prevent tooth injury, pain and discomfort. They also do grinding and polishing so that there are no burrs left on the surface, plaque does not accumulate, and the filling has a natural shine.
Classic treatment
The drilling method is the most affordable way to treat all stages of caries. In modern dentistry, drilling is used in cases where it is impossible to cure the disease by other alternative methods, for example, with medium and deep caries.
Drilling out a carious lesion is usually carried out after local anesthesia, which can significantly reduce pain. After drilling, the tooth is filled, and in order to consolidate the effect of the procedure, the patient is prohibited from eating for at least one hour after the filling is installed.
In the photo, a dentist with a drill and a mirror is about to begin treating a patient.
Treatment of caries requires an individual approach. Before using the drill, the dentist must:
- cleaning the affected tooth from plaque;
- will determine the base color of the enamel. This is necessary to select the color of the filling;
- will select a drug for anesthesia. It is important to exclude possible allergic reactions;
- will remove carious tissue. This will prevent further tooth decay;
- isolates the tooth from saliva;
- At the end of the process, a seal will be installed.
Filling materials help eliminate existing defects. Installing a filling is necessary to restore the anatomical shape of the teeth. Dentists use composite photopolymer materials; they are the most durable and durable.
The table contains a description of the treatment using the preparation method.
Algorithm of actions when preparing carious cavities:
source
Complications that can occur due to improper treatment of caries
Treatment of caries may be accompanied by one or more factors that can lead to complications.
This may be faulty equipment, low-quality materials, unqualified personnel, the complexity of the anatomy of the dental organ, an inconveniently located caries cavity, and so on. The most common complications are:
- The filling has fallen out or caries has developed around it. The reason is usually poor cleaning of the cavity from pathogenic bacteria.
- Pain in a filled tooth. To get rid of caries, especially in its deep form, the doctor must carry out each point of treatment efficiently: it is enough to cool the tooth during preparation, carefully dry the dentin, place the treatment pad correctly, and so on. Pain can be caused by overheating of the tooth, overdrying of the dentin, accidental opening of the pulp chamber, lack of a therapeutic lining and other reasons.
- There is no contact point. A tooth cannot function normally if the doctor has formed poorly or not formed contacts between the tooth being filled and neighboring dental organs. At the same time, the gingival papilla is compressed and may even bleed, which can provoke periodontitis and tooth mobility.
Ultrasound removal of deposits
For the procedure, ultrasonic scalers (or scalers) are used - devices that can generate vibrations in the range of 25-50 kHz. Oscillatory movements are performed by the metal attachment of the device. Tartar removal is carried out through two processes: mechanical destruction by high-frequency waves and the release of energy from bursting air bubbles. They are formed in the flow of water, which cools the teeth and removes remaining plaque. Microbubbles destroy tartar, while they disinfect the surface of the teeth. During the procedure, the enamel and gum tissue are not injured.
The ultrasonic removal method is effective against supragingival and subgingival calculus. The procedure takes about an hour, and the effect after it lasts up to a year. The disadvantage of the procedure is pain during the removal of subgingival deposits. In this case, the procedure takes place under anesthesia.
Contraindications for the ultrasound method:
- respiratory tract diseases,
- infectious diseases in acute form,
- multiple caries and gum inflammation,
- dentures and other orthopedic structures,
- HIV, tuberculosis and hepatitis.